Ideas for mentorship in oncology for medical students and early career doctors: insights from a UK-wide oncology mentorship scheme | BMC Medical Education

Baseline characteristics
The survey response rates and career stages of the participants are summarized in Tables 1 and 2. Prior to the scheme, the most common experience in oncology among mentees was via lectures and formal teaching (n = 68, 91.9%), prior involvement in a research project (n = 21, 28.4%), oncology placement at medical school (n = 17, 23.0%), other non-oncology placements at medical school (n = 17, 23.0%), volunteering (n = 12, 16.2%) and participation in the previous cycle of the BONUS Mentorship Scheme (n = 11, 14.9%). There were no statistically significant differences in these parameters between pre-clinical students, clinical students and junior doctors, except for oncology and non-oncology placements, which were more significant in the clinical and doctor groups (Additional file 1.6).
Setting of the scheme
Information on the length of the mentorship sessions and the meeting setting can be found in Fig. 1 and Fig. 2.
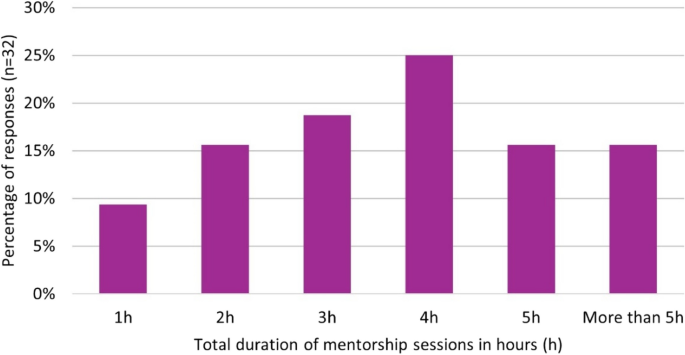
Cumulative duration of mentorship throughout the scheme as reported by mentees in the post-mentorship questionnaire
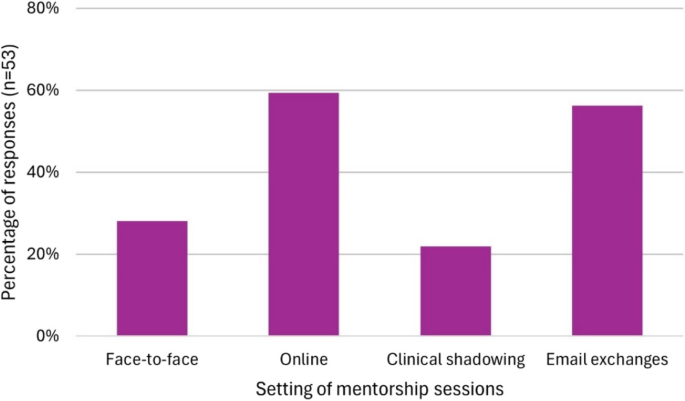
Most common setting for meetings throughout the scheme as reported by mentees in the post-mentorship questionnaire
A very small number of participants reported having some of their sessions jointly with other mentees who were allocated to the same mentor.
Knowledge of the scheme
Most mentees were interested in oncology and had specific aims and objectives for the BONUS Mentorship Scheme. Mentees’ clarity on what the mentorship scheme would look like prior to starting was divided (Table 3). There were no statistically significant differences in these parameters between pre-clinical students, clinical students and junior doctors (Additional file 1.7). Most mentors agreed or strongly agreed (n = 36, 75%) that they understood their mentees’ goals and expectations for the mentorship scheme.
In the pre-mentorship questionnaires, 78.4% of the mentees (n = 58) and 82.5% of the mentors (n = 47) agreed or strongly agreed that they would benefit from a written guide about undergraduate mentorship in oncology before starting the scheme. In the post-mentorship questionnaires, 62.5% of the mentees (n = 20) and 45.8% of the mentors (n = 22) agreed or strongly agreed with the same statement. Pre-mentorship concerns regarding the scheme were expressed in free text responses, e.g. “Having never had a mentor before, I am unsure that my mentor knows the aims of the scheme and that we may potentially become slightly unsure of the direction our mentor–mentee relationship should take.”
Expectations and motivations
A summary of mentees’ expectations can be found in Fig. 3. Most mentees expected to be involved in a research project, including audit and quality improvement. Desired oncology career advice ranged from explaining oncology career pathways to discussing specific specialty portfolio requirements. A typical response, as outlined by one participant was to “discuss with my mentor about their career and sharing ideas for how I can develop and get involved in things at medical school to help further my own career in oncology.” Another participant wished to “shadow the mentor in their daily work in a hospital setting while working with cancer cases and hear anecdotes about mentor’s experience of getting to where they are today.”
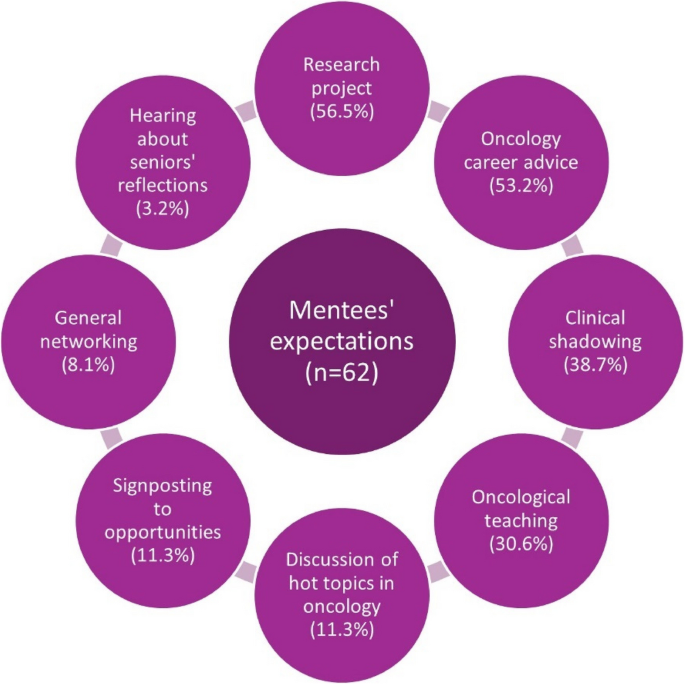
Expectations for the mentorship scheme as reported by mentees
When mentees were asked what they were most looking forward to, networking was the most frequent theme (n = 24, 38.1%). Mentees were also particularly excited to gain insight into the specialty (n = 17, 27.0%), gain research experience and outputs (n = 15, 23.8%), gain clinical experience (n = 11, 17.4%) and receive tailored career coaching (n = 10, 15.9%). Mentees generally referred to their lack of oncology exposure and therefore valued the opportunity for early experience. Mentees typically looked forward to “acquiring hands-on experience in oncology (whether clinical or research) and getting advice on how to leverage potential opportunities to pursue interest in oncology even at pre-clinical stage of medicine.”
The desirable attributes of a mentor reported by mentees are summarized in Fig. 4.
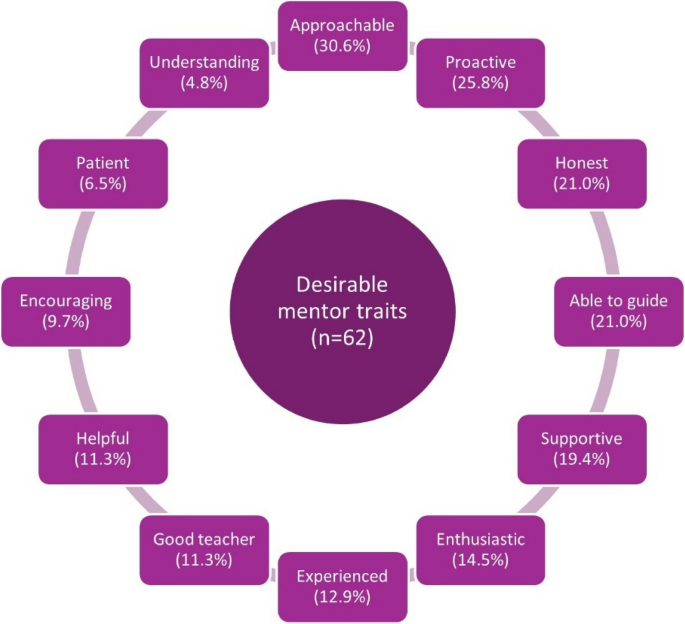
Desirable traits of a mentor as reported by mentees in the pre-mentorship questionnaire
The mentors’ main motivation to become mentors was to promote oncology or inspire students and early career doctors into oncology (n = 20, 51.3%). Other common motivations included general junior support (n = 13, 33.3%) and personal satisfaction (n = 10, 25.6%). Several mentors undertook mentoring, primarily because of their interest in medical education and to develop their teaching, mentoring and leadership skills (n = 9, 23.1%). Some mentors were motivated to improve the experience of junior colleagues due to the lack of mentorship at an early stage of their own careers (n = 8, 20.5%). Conversely, some mentors’ motivation to mentor was to “give back”, as they had a positive experience as mentees in the past (n = 6, 15.4%). One mentor reported “I have had great mentors in the past and feel that it is my time to repay it back.” Finally, a small number of mentors simply wished to form relationships and expand their network (n = 3, 7.8%).
When the mentors were asked about specific ideas for mentorship, general career advice (n = 16, 45.7%) and the desire for it to be mentee-led (n = 14, 40.0%) were the most common themes. Mentors also suggested teaching (n = 11, 31.4%), clinical shadowing (n = 7, 20.0%), research project engagement (n = 7, 20.0%) and day-to-day oncology insight (n = 6, 17.1%).
Mentors planned to develop a good mentoring relationship from the start by agreeing with expectations and plans upfront (n = 19, 52.8%), being approachable (n = 11, 30.6%), developing rapport (n = 11, 30.6%), being open (n = 10, 27.8%) and being available (n = 8, 22.2%). Some mentors also believed that an initial face-to-face meeting (n = 6, 16.6%) and clear introductions (n = 3, 8.3%) were appropriate to kickstart a good mentoring relationship. Ideas for developing rapport included inviting the mentee for a coffee and providing a reachable contact number.
The foreseen benefits of being a mentor, as reported by mentors in the pre-mentorship questionnaires, are summarized in Fig. 5.
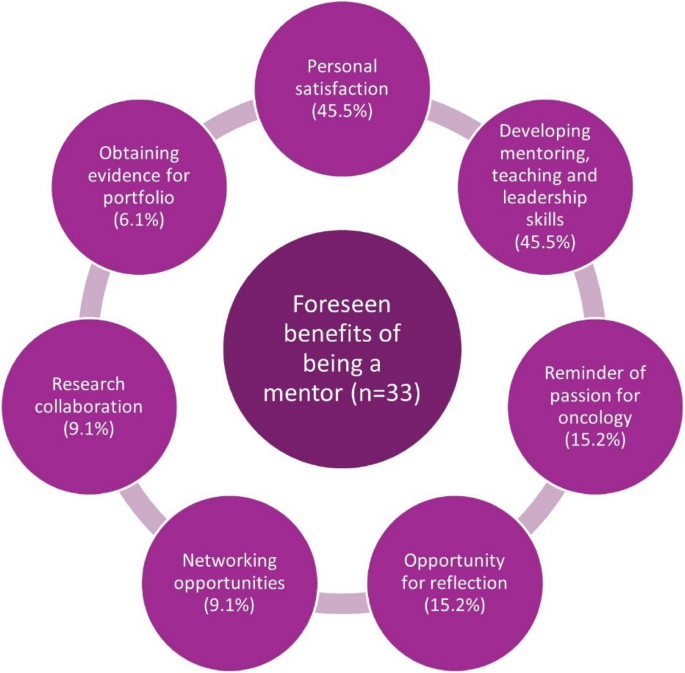
Benefits of being a mentor as reported by mentors in the pre-mentorship questionnaire
Contents of the mentorship sessions
A summary of the contents of the BONUS Mentorship Scheme 2022–2023 is summarized in Fig. 6.
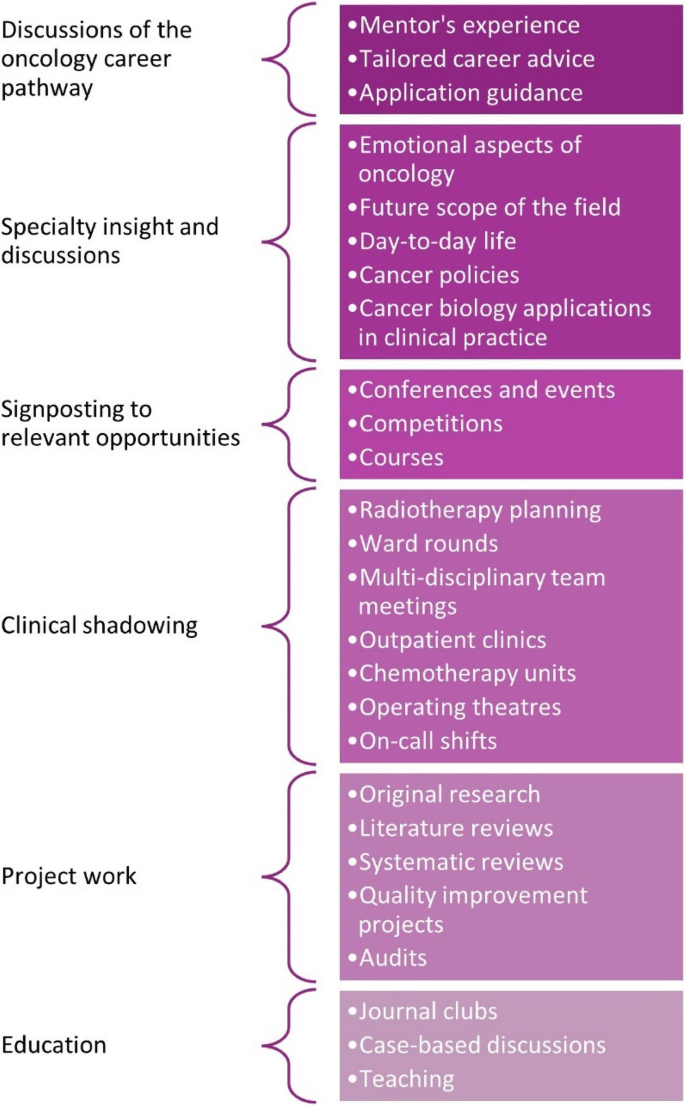
Ideas for undergraduate mentoring in oncology as inspired by the contents of the BONUS Mentorship Scheme
The most common reported content of the mentorship sessions involved discussions about the oncology career pathway (n = 12, 50.0%; n = 12, 60.0%; and n = 17, 56.7%, as reported in the first mid-mentorship, second mid-mentorship and the post-mentorship questionnaires, respectively). These included discussions of the mentor’s own professional pathway to becoming an oncologist and the lessons learned, as well as tailored career advice about the oncology training pathway for the mentees. Mentors generally offered to guide mentees in their future applications for specialty training and provided advice on intercalated degrees and study tips.
Other popular contents of the mentorship included signposting to current opportunities for mentees (n = 5, 20.8%; n = 2, 10.0%; and n = 7, 23.3%) and clinical shadowing (n = 5, 20.8%; n = 9, 45.0%; and n = 9, 30.0%). Mentees gained advice on opportunities for their training stage, such as attending relevant conferences or entering oncology-related prize competitions.
A few mentees spent their time engaging in projects (n = 4, 16.7%; n = 8, 40.0%; and n = 9, 30.0%), including research projects, literature reviews, systematic reviews, quality improvement projects and audits. A small number of mentees reported their work being published in peer-reviewed journals or being accepted for presentations at conferences and scientific meetings.
Some sessions involved discussions of oncology from a clinical perspective (n = 4, 16.7%; n = 7, 35.0%; and n = 8, 26.7%), during which medical students learned about the application of cancer biology in clinical practice. This approach was reported to be particularly valuable to pre-clinical students, who lacked clinical experience or knowledge.
Other mentorship sessions consisted of journal clubs (n = 2, 8.3%; n = 2, 10.0%; and n = 5, 16.6%), case discussions (n = 2, 8.3%; n = 3, 15.0%; and n = 5, 16.6%) and oncological teaching (n = 3, 12.5%; n = 6, 30.0%; and n = 4, 13.3%).
Teaching covered various topics, including cancer screening, oncological presentations, overviews of the cancer multi-disciplinary team meetings, oncology scoring systems, indications for chemotherapy and radiotherapy, immunotherapy, nutrition in oncology, overviews of cancer services in the National Health Service, oncological emergencies, acute oncology and evidence-based medicine.
Individualized sessions that mentors offered included summer research placement advice, doctoral degree application advice, help with an essay prize submission, planning a talk for a university society, attending a career evening and general pastoral support.
The mentor’s responses to the question about the specific content of their mentorship sessions in the post-mentorship questionnaires did not differ significantly from the answers provided by the mentees. For mentors, the most common content of the sessions was providing career advice (n = 21, 55.3%), followed by providing an opportunity for research (n = 20, 52.6%).
Nearly half of the responses described how the mentorship sessions provided the mentees with insight into oncology as a specialty (n = 17, 44.7%). This was done in a variety of ways and included discussions on the emotional impact of oncology, analysis of the future scope of the field, insights into day-to-day activities and a model weekly timetable, details of the medical and clinical oncology training programmes, and discussions of current cancer policies.
Several mentors provided clinical exposure for their mentees (n = 7, 18.4%), which included observing radiotherapy planning, attending clinics, and shadowing ward rounds and on-call shifts. Multiple mentors taught concepts to mentees during their sessions (n = 6, 15.8%), including introductions to radiotherapy, modes of action of chemotherapy and targeted therapy, as well as basic treatments for renal and colorectal cancers.
Other individualized sessions reported by mentors consisted of specific case discussions, critical appraisals of research papers and discussions of current issues in oncology.
Feedback from participants
Mentee-reported outcomes after participation in the BONUS Mentorship Scheme are presented in Table 4. There were no statistically significant differences in these parameters between pre-clinical students, clinical students and junior doctors (Additional file 1.8).
Mentees and mentors reported online meetings to be the most useful (n = 19, 59.4% of mentees and n = 21, 43.8% of mentors), followed by face-to-face meetings (n = 6, 18.8% and n = 13, 27.1%) and clinical shadowing (n = 5, 15.6% and n = 6, 12.5%). There were no statistically significant differences in these parameters between mentees and mentors at different stages of their careers (Additional file 1.9). Email exchanges were reported to be the least useful by both groups (n = 10, 71.4% of mentees and n = 19, 39.6% of mentors).
Mentees generally strongly agreed or agreed (n = 16, 50.0%), 37.5% (n = 12) were neutral and 12.5% (n = 4) disagreed that they would have benefited from pre-arranged meetings with fellow mentees to share ideas. In terms of mentors, 35.3% (n = 18) strongly agreed or agreed, 47.1% (n = 24) were neutral, and 17.6% (n = 9) disagreed or strongly disagreed that they would have benefitted from prearranged meetings with fellow mentors to share ideas. There were no statistically significant differences in these parameters between mentees and mentors at different stages of their careers (Additional file 1.10).
Most mentees would have preferred to be part of the mentorship scheme during the clinical years of medical school (n = 23, 74.2%). Mentees generally plan to stay in touch with their mentor beyond the official timeframe of the scheme (n = 27, 84.4%), as so do mentors (n = 38, 79.2%). A total of 95.7% (n = 45) of the mentors would recommend their colleagues to become involved as mentors in the scheme and 95.8% (n = 46) would join the scheme again. There were no statistically significant differences in these parameters between mentees and mentors at different stages of their careers (Additional file 1.11).
In the post-mentorship questionnaire, mentees most commonly referred to overall exposure to oncology as a benefit of the scheme (n = 10, 40.0%). Other benefits included confirmation of oncology as the right future career choice (n = 7, 28.0%), having a future career plan and resources (n = 5, 20.0%) and gaining invaluable research experience (n = 5, 20.0%). Mentees described benefitting from new knowledge, new or additional clinical experience, detailed career discussions and networking opportunities. As an example, one mentee described the benefits as “having more of a concrete idea about clinical oncology and plans to go down this route as it has all the elements I value in a career (research, clinical time, work/life balance)”.
Mentors stated that research experience (n = 12, 34.3%) was one of the key benefits of the scheme for the mentees. Career building (n = 9, 25.7%), discussions of what a career in oncology is like (n = 9, 25.7%) and gaining specific specialist knowledge of oncology topics were also perceived benefits for the mentees. A few mentors believed that specialist clinical experience (n = 4, 11.4%) and networking (n = 3, 8.8%) were the main benefits for mentees. For example, one mentor described that their “Mentee near end of medical school was able to attend an oncology careers evening I helped organise and signposted her to. I also gave networking and research opportunities with local oncologists.”
Most mentors reported that personal satisfaction (n = 16, 48.5%) was the main benefit for them. Mentors also believed that the scheme promoted oncology as an attractive career choice for students and doctors (n = 6, 18.2%). For some mentors, reflection on their career as oncologists (n = 4, 12.1%) and the opportunity to develop their mentoring (n = 3, 9.1%) and teaching (n = 2, 6.1%) skills were the key acquired benefits. One mentor described: “The inquisitive questions asked by the mentees always make me reflect on why I chose oncology and in a busy and pressurised time, help me to remember all the things I love about it!”.
There were no specific areas of the mentorship scheme with which the mentees were dissatisfied. Individual responses for the areas of improvement included having better communication from the mentor, having more research and clinical shadowing opportunities, meeting face-to-face as opposed to online, having meetings more frequently and increasing the duration of the scheme. Many mentors referred to their own time constraints as the main obstacle of the mentorship scheme (n = 18, 48.6%). Some mentors reported that a lack of sufficient time, logistical issues in setting up access to systems and a lack of experience from students were obstacles to conducting research.
link





