A theory of change approach to curricular revision: filling a curricular gap identified through curriculum mapping | BMC Medical Education

At the start of our curriculum mapping efforts in 2018–2019, we did not anticipate identifying any specific gaps in our UME curriculum and were surprised to realize how few of our session-level learning or course objectives (and assessments) related to prognostication. Previous reviews of our UME curriculum by faculty and students had not identified this topic as an area of deficiency for our learners, suggesting that the experienced (or learned) curriculum was adequate on this topic. Nonetheless, our intended (written) curricular session-level learning objectives did not provide evidence that our students mastered this competency. Mismatches between the intended (planned or written) curriculum, the delivered (taught and/or tested) curriculum and the experienced (learned) curriculum can occur whenever instructor goals, classroom instruction and assessments, and student perceptions of curricula do not align [19, 20].
Correcting misalignments and/or gaps in a curriculum map is essential if all stakeholders, including curricular oversight bodies and accreditors, are to have an accurate and shared understanding of what the curriculum includes and how it is sequenced. Moreover, a robust curriculum map facilitates the process of identifying how new topics can be included in an existing curriculum. Sullivan and colleagues, for example, leveraged a curriculum map at their own medical school to propose how new curricular content on climate change could be added to existing curricular sessions without increasing curricular time [21].
Although some authors have criticized Theory of Change models as overly linear [22], this linearity can be helpful when considering complex systems. Utilizing the ToC approach for curricular revision prompted us to recognize our fallacy in assuming there was good alignment between our curriculum map and our educational goals. Moreover, it helped us to strategize how best to fill the gap in our curriculum map by guiding us in identifying specific resources that were available for correcting this misalignment, including opportunities for learning and assessment within our curriculum, and curricular leaders who could be tapped to help. Other authors have reported finding and filling a curricular gap without specifying how they decided on the specific curricular interventions or how they implemented curricular revision. For example, Fisher and colleagues proposed including Interprofessional Education (IPE), simulation and e-learning pedagogies in a UK medical school curriculum to address a curricular gap on the topic of delirium, but did not explain why they thought these teaching strategies would be best [23]. Similarly, a report that identified a gap in substance misuse teaching at 19 medical schools in England did not describe how or why the authors decided on specific learning outcomes or curricular materials in order to fill the gap [24].
Utilizing a Theory of Change model for curricular revision has the advantage of requiring curriculum designers to articulate reasonable short-term and medium-term outcomes that would measure progress toward curriculum revision. Our outcomes included curriculum committee approval of new course objectives in Phase 2 and 3, and confirmation that student performance on prognostication is assessed on the evaluations associated with clinical courses in Phase 2 and 3 (see Fig. 4). Identifying and listing the anticipated outcomes of curricular revision makes the process of transparent to stakeholders. Given that many curricular reforms at medical schools meet with inertia and resistance [25], communicating how curricular revision will be measured is critical. Facilitating the buy-in of stakeholders is an essential element of any successful change effort [26].
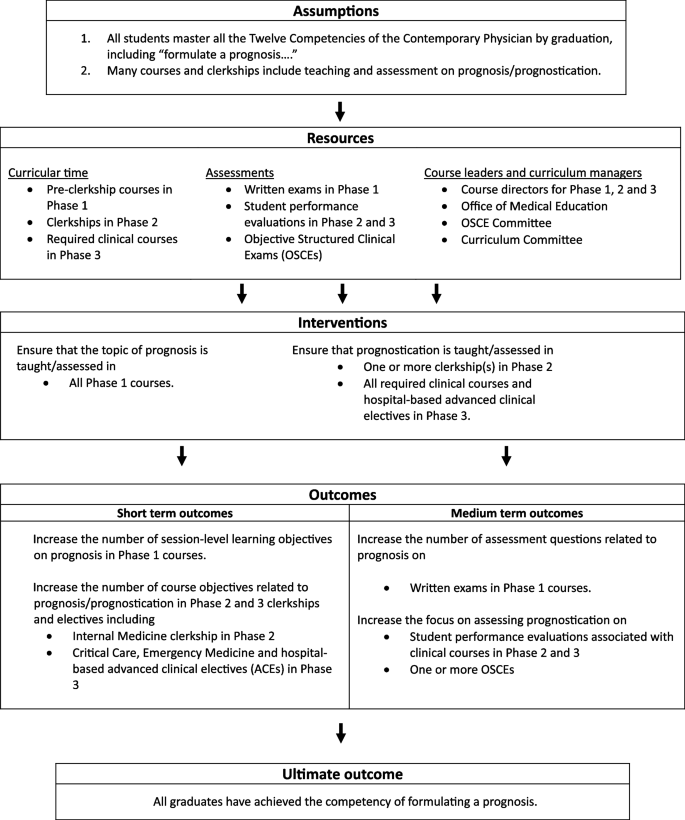
Theory of Change framework for curricular revision to address a curricular gap on prognostication. The framework requires specification of any underlying assumptions about the existing curriculum design (i.e., the need for change), the resources available for curricular revision (i.e., the personnel, curricular time, and testing materials necessary to effect change), the curricular interventions that would fill the identified curricular gap (i.e., the strategies for effecting change), and the short-term, medium-term and ultimate outcomes or indicators expected from revising the curriculum (i.e., the benchmarks for measuring change)
In summary, utilizing the structured Theory of Change approach to implement curricular revision has several advantages. First, the ToC methodology requires that the assumptions underlying a curriculum and the corresponding curriculum map be made explicit. As described above, this requirement can provoke new realizations on the part of educational leaders about the design of an existing curriculum and its curriculum map. Second, developing a ToC model prompts curriculum designers to list multiple interventions that might be appropriate for revising the curriculum. This strategy discourages any temptation to jump to conclusions on quick fixes to “patch”, and superficially correct, curricular gaps. Thirdly, the ToC framework requires that short and long-term outcomes be articulated to specify how progress towards the long-term goal of curricular revision will be measured. This step clarifies, in a manner transparent to all stakeholders, how curricular change will be recognized and documented. The ToC framework also can be used at the classroom level to understand the effects of individual education experiences [27].
The authors acknowledge that it is a limitation of this report that we describe evidence of a curricular gap based on a lack of learning objectives on the topic of prognosis and prognostication. We did not consider the degree to which the curriculum did or did not include assessments of these topics. However, as the policy at our institution is that all assessments must be linked to learning objectives, it is unlikely that significant assessment of prognosis/prognostication took place in the absence of learning objectives. In addition, it is a limitation that we report outcomes from using the Theory of Change model to effect curricular revision at one US medical school. Nevertheless, as the approach could be used to correct curricular gaps of any type within educational programs of any scale, we report our experience in hopes that the ToC approach might be of interest to educators those who oversee and design health science curricula at other schools.
link